Introduction
We are afraid of what we don’t understand. Mental illness is an issue that is so cryptic and nuanced in nature that it scares us.
Anxiety and depression, as Clayton High School juniors Kayley*and Charlotte* illustrate, are but two of the myriad of psychological issues facing millions of Americans annually.
Clinical psychologist at Family Life Counseling and Psychological Services Susan Sanderson explained, “Everyone has felt sad at one time, but when the sadness becomes something that impairs functioning and sleep and appetite and energy, that’s when it can be defined as a mental illness.”
-•–•–•-
“You can’t breathe. It’s like an asthma attack, even though I’ve never had an asthma attack. It’s like you’re always in your head. You’re thinking constantly about yourself. Racing thoughts.”
– Kayley*
“It’s like you’re constantly being weighed down by something. When you’re depressed, [it’s like] you’re in the middle of an ocean. You have no idea where you are and you’re just treading water and you’re just so tired of treading water. When you start recovering, you start floating and then you just pick a direction and start swimming. You’re so tired and it’s so hard, but you just have to keep swimming. And eventually, you find a boat, but it’s a really shitty boat and it’s always leaking and you have to keep dumping [water] out. Even when you’re “better”, you’re still in a pretty sucky place. You get so used to just being sad. And when you’re actually completely happy, it’s the most amazing thing in the world and you just want to pause. You just want to take a remote and pause. You never feel this feeling of happiness and then it just goes away in an hour or even less.”
– Charlotte*
*Asterisk indicates the name and identifying details have been changed to protect the privacy of the individual.
The Factors
Similar to many other diseases, mental illness is rooted in biological components.
St. Louis University Psychiatrist Anjan Bhattacharyya explained, “[Mental illness] is a complicated story that is being studied a lot now. We know that there are certain areas of the brain that are not functioning well with depression or anxiety. For example, a lot of people with anxiety have panic attacks, so the amygdala is overactive. For people with depression, the temporal lobes and what we call the limbic system is deeply involved, especially in areas such as the anterior cingulate cortex.”
A wide variety of neurotransmitters, such as serotonin, epinephrine and cortisol play an integral role in the brain chemistry aspect of mental illness. However, the issue is not always so black and white.
“I often think of it as a three-hit hypothesis: there’s the genetic, early life component and the acute stressor. So clearly genes play a big role,” Bhattacharyya said. “If you have a first degree relative, especially a parent, with depression or anxiety, it significantly increases your ability of developing depression or anxiety.”
Despite the progress that has been made over the past few decades in shedding light on the causes, biological and environmental, of mental illness, there is still a long way to go.
“I think that right now, we are really on the cusp of learning how the mind-body connection works and what all the risk factors are,” Sanderson said.
In addition to the aforementioned biological contributors, environmental influences also impact the development of mental illness.
“Every time I see something, smell something, hear something, it affects my brain. Similarly, it’s not just those primary senses, it’s putting them together in a sociocultural context,” Bhattacharyya said. “It’s really an interplay of internal things that are determined by genes and maybe chemistry and external influences such as how you were raised, what kind of diet, what kind of activity you’re in. All of those things impact your mental state at the time.”
A diagnosis for a mental disorder is not as straightforward as other illnesses because there is no one identifying test. “Mental illness is defined by society, so it’s not something that there are blood tests for or DNA tests for,” Sanderson said. “It is defined by what seems to be normative in our society and what is considered to be abnormal; specifically, what’s considered to be functional and what’s considered to be impairing functioning.”
Oftentimes there is a misconception in society that all people with mental illnesses must have experienced a tragic backstory or loss prompting the development of their illness.
“Sometimes the environmental stressor can be something pretty significant like abuse or neglect,” Sanderson said. “Sometimes it can be something like divorce or a learning disability that causes the child to be bullied, or something like that. It doesn’t have to be what most people would consider a large stressor to trigger it for people.”
Psychologists, like many other researchers, are still uncovering the many phenomenons associated with the science they study. But there are still questions left unanswered.
“I don’t think we know yet what fully causes depression and anxiety and what the triggers are,” Sanderson said.
Although there are many forms of mental illness, the two forms most frequently seen in our society are anxiety, impacting the lives of 18.1 million American adults and depression, affecting 15.7 million.
“I think that anxiety and depression are more common because they are affected by all aspects: the social aspect, the genetic component, the physiological aspect, all of those things,” Sanderson said.
Personal Stories
CHS students and teachers share their stories regarding mental health.
Lauren Compton Nate
Grant Friesen Kamal Lado
Charlotte Rebecca
John Layla
Kayley Rachel
Sydney Danielle
Jason Megan
Madison Meredith
Ann Emily
Amanda Barbara Dobbert
Annabelle Maria
*Personal stories as told to Alex Bernard, Camille Respess and Ellie Tomasson were edited for content
The Stigma
stigma / stig•ma n. a set of negative and often unfair beliefs that a society or group of people have about something (Webster).
-•–•–•-
Depression is a sign of weakness. Anxiety is sign of instability. Mental illness is something you just need to buckle down and power through.
According to Sanderson, these sentiments are echoed throughout our society.
“We, as a society, unfortunately tend to view mental health issues as completely under the person’s control,” Sanderson said. “So we see it as a sign of weakness if they don’t ‘get it all together.’”
When someone breaks their arm, no matter how strong their power of will, they cannot fight the healing process and recover promptly. Although not widely acknowledged in society, dealing with a mental ailment is very much the same.
“I think [the stigma] inhibits people from getting the help that they need because they don’t want to be seen as weak or they don’t want to be blamed,” Sanderson said. “Once they come to therapy, they usually feel very empowered because they can learn that this isn’t their fault, they didn’t ask for it, it’s not a character defect and they can learn ways to help manage it and get better.”
Similarly, Bhattacharyya finds the ignominy in common culture regarding mental illness to be problematic.
“As much as we have progressed, it’s still for the vast majority of people, quite crushing to admit or seek help for a mental health problem that needs help. That’s something that we call stigma and it’s a big player in preventing people from getting help,” Bhattacharyya said.
The way that mental health, specifically depression, is portrayed in media is a large factor in how it is viewed in common culture.
“There’s a stigma with [depression] and you see it in TV shows where they’re like all sad and emo and wear all black. I mean I do wear all black but that’s just because I like the way I look. It’s just seen as this negative thing,” CHS junior Kamal Lado said.
Additionally, misconceptions exist around the vitality and abilities of a person with depression.
“[People think that] if you are depressed, then you are weak and that it is embarrassing,” CHS junior Madison* said. “You must be really bad at things if you are depressed. Your life must suck if you are depressed.”
Due to this mentality of inadequacy, many avoid confronting mental illness in order to maintain their flawless facade. When people are forced to deal with their mental illness, they have to acknowledge their perceived imperfections.
“It’s a concern for me knowing the stigma surrounding mental health and that it is just something that you don’t talk about, it’s pushed under the rug,” CHS teacher Lauren Compton said. “Frankly, I think that people are afraid to talk about it because it will bring up issues and may make people upset.”
These issues reinforce the perception of ineptitude that accompany the inability to properly address psychological health concerns.
“I think that it’s something that many people can talk about very briefly and touch on, but actually sharing personal mental health experiences is not only taboo, but also still makes people very uncomfortable. I know that personally makes me very uncomfortable,” CHS junior Harper* said.
On a superficial level, mental health can be discussed, but when it comes to making oneself vulnerable and sharing personal struggles, the dialogue often fizzles out.
“It is something that is pretty much kept hidden unless you really open up to somebody else,” CHS junior John* said. “But it is not something that people bring up on a day to day basis. It is like a rare topic of discussion.”
When a wolf strays from the pack, it is left to fend for itself. Similarly, human nonconformity induces ostracization from the greater society.
“Having a mental health disorder is abnormal from not having one. Already, that sets you apart. Most people really don’t like being set apart. They’d rather be with the rest of the people,” CHS junior Grant Friesen said. “When you set them apart, they feel isolated and different. Really though, we are all just people, we all just work differently.”
Mental Health in Clayton

According to a survey given to 216 CHS students, 40.74 percent of students have personally struggled with issues of mental health.
67.37 percent of CHS students have a close friend or family member that has struggled with issues regarding mental health.
Mental health touches the lives of the majority of the student body at CHS, in some form. In this reality, CHS grade level counselor Tobie Smith believes that Clayton provides opportunity to talk about this subject.
“I think in terms of how [mental health] is discussed, it’s very open and accepting in all kinds of areas,” Smith said.
60.75 percent of CHS students feel that they can talk to their peers about mental health issues.
“I have instances where I have people who are close to me, but I haven’t really told [about my depression] come to me and say like, ‘If you need anyone I’m here’ and I’ve had that with most of my friends and that’s always really great to hear,” CHS sophomore Sydney* said.
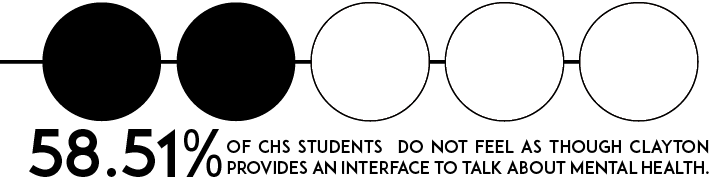
However, this means that 39.25 percent of students do not feel that they are in a position to have conversations about this topic.
“I’d say most people I wouldn’t feel comfortable opening up to because a lot of people here especially are just rude or ignorant and don’t care or don’t know what to say,” CHS senior Nate* said. “Maybe that’s just the experience that I’ve had with people in general, not everyone is like that. But here, I’d say, most of the kids, there’s been issues with that.”
Moreover, the shame that students may feel about their mental illness can attribute to the silence regarding this topic.
“Personally, I feel that something is wrong with me,” CHS senior Ann* said. “I feel that people are judgy and they don’t take things that seriously and it turns into, ‘Oh she’s just trying to get attention,’ or, ‘She just thinks she feels that way and doesn’t know how you’re supposed to feel.’”
The judgement that students at CHS may sense regarding many topics plays a pivotal role in what feelings they choose to expose and which ones they do not.
“You can’t just show up to school sad all the time because no one’s going to want to be your friend, and you’re looked at differently, so you have to tie it all up, and put it in your stomach, and put a good face on and pretend like nothing’s wrong,” CHS senior Emily* said.
During a semester long health class for sophomores, the topic of mental health, specifically depression and suicide, is studied for a two week long period.
48.94 percent of CHS students feel that Clayton educates its students well enough about mental health issues, leaving 51.06 percent feeling otherwise.
“Clayton tries so hard to teach people how to deal with friends who are depressed,” Charlotte said. “And, honestly, they don’t do it very well.”
This lack of understanding can stretch throughout the classroom experience for students. When a student has the flu, they inevitably miss class time during recovery. But when a student has a mental illness, missing school due to that becomes much more complicated.
“I can’t afford to skip any days of school because of this [depression]. It’s not going to be understood in Clayton, like, ‘You missed school because you were sad?’ No one’s going to understand that,” Charlotte said.
CHS is an academically focused environment. For Charlotte, the pressure to do well in school and also live with her depression has created difficulty in her life.
“In Clayton, your whole life becomes school, like revolved around school because there’s so much pressure to be amazing. So much pressure to be a genius,” Charlotte said. “If something happens that takes your life from being completely revolved around school, it’s like what are you going to do? You can’t do anything. You just want to go home and die. You have to force yourself to go on.”
CHS senior Megan* has avoided discussing her mother’s depression to avert showing her peers that her life involves emotional challenges.
“There’s the pressure to just seem like you’re doing fine all of the time and you’re handling all of the stress and you’re doing really well,” Megan said. “That’s sort of what you’re supposed to do at Clayton, like, be perfect. So, I guess that made me not want to talk about it with the people at Clayton. I wanted to seem like I was doing fine and everything was okay.”

Counseling Department

The counseling department at CHS can be seen as a haven for students to open up about their lives. 62.77 percent of CHS students feel that they can talk about their personal life and struggles with their grade level counselor. But for 37.23 percent of the student body, talking about the intimate details of their life with their counselor is not something they feel comfortable with.
“I don’t really feel like I can talk to my counselor because I see our relationship as academic, the only things that I talk to her about is my schedule. Unless I establish a relationship with her where I can talk about personal things, I don’t know if I could ever really feel that close to her in that way,” CHS junior Danielle* said.
In addition to being a source for students to talk about their personal life, the counselors at CHS also have academic responsibilities including scheduling, planning standardized testing and aiding students in the college process. But student needs are at the forefront of their attention.
“Our primary focus is our students and if a need presents itself, basically everything else takes a back seat to that issue,” CHS grade level counselor Alice Morrison said.
Opting out of discussing mental health issues with a grade level counselor, for some students, is rooted in their desire to avoid bringing their personal struggles into their academic environment.
“I love Ms. Bell so much. I think she’s really wonderful, but I would rather keep those things very separate. I felt more comfortable keeping it very separate. Like, school and mental health issues,” Harper said.
Morrison understands the existence of this rationale.
“We don’t have to know the problem, we don’t have to understand every aspect of it because some students don’t want to blend those two worlds, they don’t want to blend their academic world with their social, emotional life,” Morrison said.
Similar to Harper’s desires, Charlotte lacks both the ability and inclination to go to the counseling department for help with her depression during the school day.
“They [the counseling department] seem like nice people. I feel like if I went to them, it’d be like bringing my issues into school. I can’t miss a class because I don’t have a lunch period to just go talk to them about that,” Charlotte said. “I feel like 45 minutes isn’t enough.”
Charlotte also does not feel secure with talking about her depression with her counselor at CHS, in part, because of the discomfort she felt doing so in the past.
“In middle school, I saw the school counselor a little bit and honestly, it didn’t really help me that much because you were seeing them in the hallways walking by you and it’s like, this person knows really, really intimate details about me. It’s weird because you see them all the time. I barely know them. I don’t feel close to them at all,” Charlotte said.
But the counseling department does strive for students to see their offices as a place to speak freely about their lives.
“A large majority of our job is how we welcome students, we hope that we create an environment that is welcoming to students where they could step in here and talk to any one of us and feel like they’re being heard,” CHS college counselor Mary Anne Modzelewski said.
In CHS junior Amanda’s case, she has been able to do so.
“They have helped me. I cannot speak about other people because I just don’t know, but they have helped me a lot to understand what I need to do if I am every feeling anxious and having a panic attack. It is a comfortable place for me to talk about how I feel,” Amanda said
In Sanderson’s opinion, high school counseling departments in all of society can do a better job in being a place where students can feel secure.
“There is certainly room for improvement [within high school counseling departments]. They are the first responders, so it would be good if they presented themselves as more warm and open,” she said.
For some students, their reasoning behind not reaching out to the counseling department about their mental illness may simply be their unfamiliarity with knowing that that is a possibility.
“Our grade level counselor is nice. I don’t know if I would feel comfortable talking to her though,” Kayley said. “I don’t know what it is.”
This level of unawareness can point to the reality that students often perceive the counseling department to be academic based.
“When I think of the counseling department here I think of college and changing your class and stuff so I think that maybe, possibly, if we had a counselor that was just dedicated to more of therapy and getting your feelings out I feel that that would make a tremendous difference,” Rachel said.
Grade level counselor Joyce Bell believes that the impression some may have of the department being focused strictly on schooling has to do with the times in which the counselors interact with the student body on a larger scale.
“You see us when we’re in your classroom about testing, you see us when we’re in your classroom talking about registration, you see us when we’re in your classroom talking about careers,” Bell said. “So that’s in your mind and it’s all academics, but we do the personal stuff too. Probably more than all of those other things, but that’s not what is seen on the outside and we need to get that message out there.”
For some students, reaching out to the counseling department about their mental illness can create uneasiness. In Madison’s view, student’s lack of knowledge in regards to how much the counseling department can help is one of its greatest pitfalls.
“I think that the counseling department is really good at helping kids when they need it. But they don’t make it known that kids can come to them whenever. When you do get in there and get help, they are really effective. But if you didn’t know that, then no one would ever know,” Madison said.
But some students have had beneficial interactions with their counselors about mental illness within the walls of CHS.
“Ms. Bell is pretty much my therapist. I know that I can always go to her if I have a problem. When I am having a panic attack and she is available, she knows what to do. We go for a walk around the school or something like that and I will relax,” Amanda said.
Likewise, Nate has been able to work through the challenges mental illness has posed him with the assistance of the counseling department.
“Just a couple days ago I got called into the counseling department. I went in there and I talked to Mrs. Morrison for a while,” Nate said. “She was really supportive, she was just awesome. She knew what to say. Definitely the counseling department has helped a lot, just being there for me and wanting to check in on me.”
Prescription Process
 There exists a commonly believed fallacy that psychiatrist and psychologist are synonymous. However, there is a significant difference.
There exists a commonly believed fallacy that psychiatrist and psychologist are synonymous. However, there is a significant difference.
“Psychologists focus on the non-biological aspects of the brain and the mind. So psychologists train and have an understanding of functionally how the brain works,” Bhattacharyya said. “Psychiatrists are medical physicians, so they are trained in medicine. They understand the biological part of how the brain works as well as the mind side of it. Psychiatrists treat people with medication and some also do talk therapy.”
Both professions, however, involve interacting and treating people with mental illness. Additionally, both have the ability to diagnosis patients with mental illness.
The diagnostic process involves delving into the symptoms that a patient may be feeling, how long they have been feeling this way and what has been going on in their lives to create such a feeling. Since this approach requires patients to discuss what’s going on inside their head, it can pose some difficulty.
“It’s hard for people to describe what they’re feeling and thinking. So it takes a little bit of training to learn how to tease those things out,” Bhattacharyya said.
Although the symptoms correlated with depression can differ, there are some signs and symptoms that assist professionals in diagnosing their patients.
“For depression, you would not only see sad mood or irritable mood, you would also see difficulty sleeping, difficulty eating, lack of motivation, low energy, feelings of helplessness, feelings of hopelessness, worthlessness and sometimes thoughts of death or suicide,” Sanderson said.
Whereas in terms of anxiety, the symptoms can involve a person feeling so anxious that it impairs their daily functionality.
“They stop doing the things they need to do, like they start avoiding going to school because they are so anxious,” Sanderson said. “They may begin starting to have panic attacks where their heart is racing and they can’t breathe, they get sweaty and shaky. So they stop doing things to avoid these feelings.”
One of the greatest challenges for psychiatrists is the ambiguity that exists in their profession, this is especially present in the diagnosis and prescription process.
“It’s not an exact science. So we can’t necessarily say that if a person comes in with symptoms of depression, this is the medication that will help,” Bhattacharyya said. “We can say that these are several medications that may help the person and then there is a bit of a process of trial and error where the psychiatrist will work closely with the person to find out what is best for them.”
For many patients, hesitancy to begin taking medication for their mental illness can exist due to a variety of factors including the fear of dependency and shame they may feel for needing the medication to live as they wish.

“It is a really strong dependency. The medicine works really well but at the same time you don’t want to have a strong dependency on medicine,” CHS senior Rachel* said.
But for some, apprehension may not occur due to the desire to repress the symptoms of their mental illness.
“I kind of make fun of it myself and say, ‘These are my crazy pills, they keep me calm’, but it really does,” Compton said. “I wasn’t hesitant about taking medication because I just did not like the way I felt without it.”
Similarly for CHS math teacher Barbara Dobbert, the impact of being on medication for her depression is immense.
“Before I was put on medication I just didn’t feel like my normal self. It was an effort to do laundry and make dinner for my family or go to the grocery store,” Dobbert said. “I’d come home and all my energy would be spent at work and I would just be a blob on the couch and my mom said, ‘This isn’t you Barbara, what’s going on?’ I was depressed and it took awhile to find the right medication, but I feel amazing now.”
Although medication can be very effective for many people, due to the stigmatization of mental illness in society, some feel the need to hide the fact that they are on medication.
“My siblings don’t even know that I’m on medication. I hide it from them in my bathroom,” CHS senior Emily* said. “I don’t tell any of my friends. It’s very uncomfortable to talk about, even with my parents, [even though] I have to.”
Impacts
“I’ve appreciated more day to day things. It’s kind of like a close brush with death where you realize how much you have to be thankful for. I was on the road to suicide. The biggest lesson I’ve learned is that everything is temporary and that all your states of minds, your feelings are temporary. They may be absolutely awful, totally uncomfortable but it’s going to go away and there’s going to be a better side to things.”
– Meredith
“It is defined by what seems to be normative in our society and what is considered to be abnormal; specifically, what’s considered to be functional and what’s considered to be impairing functioning.”
– Susan Sanderson
“It’s a concern for me knowing the stigma surrounding mental health and that it is just something that you don’t talk about, it’s pushed under the rug. Frankly, I think that people are afraid to talk about it because it will bring up issues and may make people upset.”
– Lauren Compton
“Having a mental health disorder is abnormal from not having one. Already, that sets you apart. Most people really don’t like being set apart. They’d rather be with the rest of the people. When you set them apart, they feel isolated and different. Really though, we are all just people, we all just work differently.”
– Grant Friesen
-•–•–•-
Mental illness has a ripple effect; it reaches farther than the individual and affects the people closest to them. These reverberations can manifest themselves in different ways.
“It affected my relationships with my friends and my family primarily. My family, I think, lost some trust in me,” Harper said. “Not only did I do things during that time that they weren’t comfortable with me doing, but additionally, now, every time I’m upset, they freak out a little bit and it makes things kind of a strain.”
In some instances, family members are not able to comprehend what it’s like to live with mental illness.
“My dad absolutely hates [my panic attacks]. He yells at me. I wouldn’t want to say that he thinks they’re bullshit, but he kind of does. I just kind of feel like he doesn’t really understand,” Kayley said.
This inability for friends and family to accept mental illness can cause them to ostracize the afflicted.
“I have had friends that have told me that they don’t know how to deal with this so there are situations where I don’t get included anymore because they are afraid that I am going to have another anxiety attack or episode,” Compton said.
For some, their mental illness has caused them to disconnect from the social aspects of their lives.
“I lost a lot of friends just because I think I was kind of isolating myself, the dynamic of the relationship changed and I’m still feeling the different dynamics of friends I’ve had in that period or throughout that time because they still think that they have to take care of me even if I don’t feel like I need to be taken care of any more,” Harper said. “You still feel that dynamic of helper and helpee.”
Moreover, the way that relationships can alter cause people with mental illness to feel not only that they are being looked after by their friends, but also that they cannot have the same dialogues with their friends as the ones that they may have had in the past.
“People treat you like you’re made of glass or like they’re constantly walking on eggshells around you. I don’t want you to think about everything before you say it,” Charlotte said. “I still want to joke around with people without them thinking constantly about my feelings. I still want people to do that dumb banter between friends.”
Even outside of the circle of close friends and family, mental illnesses affect the relationship of the individual to the greater society.
“Whenever I have panic attacks in school or in public, I always feel like everybody is looking at me,” Kayley said. “If I’m in public, I feel like everybody is looking at me. Everyone is judging me. And I can’t get these thoughts out of my head. It’s just a cycle of thoughts. It’s like “you’re stupid. You’re dumb. This whole thing is dumb. Nobody likes you.”
Although these mental ailments can negatively affect the life of the individual, they can also be used as opportunities for personal growth.
“I’ve appreciated more day to day things. It’s kind of like a close brush with death where you realize how much you have to be thankful for. I was on the road to suicide,” CHS senior Meredith* said. “The biggest lesson I’ve learned is that everything is temporary and that all your states of minds, your feelings are temporary. They may be absolutely awful, totally uncomfortable but it’s going to go away and there’s going to be a better side to things.”







